Most people use the word “credentialing” to mean all of it: the applications, the approvals, the contracts, the directory listings. In practice, those are separate steps, and understanding how they fit together helps you plan better and avoid surprises.
Credentialing
Credentialing is the process of verifying who a provider is. It confirms that a provider’s education, training, licenses, and work history are accurate and current.
Every payor runs some version of this before they will allow a provider to participate in their network. It is also required by hospitals, health systems, and accreditation bodies, though the focus here is on the insurance side.
Credentialing answers the question: is this provider qualified and compliant?
Enrollment
Enrollment is the process of getting a provider or practice officially registered with a specific payor or plan. It is sometimes called payor enrollment or provider enrollment.
Where credentialing is about verifying who you are, enrollment is about formally joining a network. A provider can be credentialed and still not enrolled with a specific payor. Both have to happen before claims will be paid.
Enrollment answers the question: is this provider officially registered with this plan?
Contracting
Contracting is the agreement between the practice and the payor that sets the terms of participation: what services are covered, what the reimbursement rates are, and what the rules are for billing and compliance.
In many cases, contracting is tied to enrollment. When you enroll with a commercial payor, you are typically also agreeing to their fee schedule and participation terms. In other cases, especially with larger groups or multi-specialty practices, contracts may be negotiated separately.
Contracting answers the question: under what terms are we participating?
Directories and effective dates
Once credentialing, enrollment, and contracting are complete, a payor updates their provider directory to reflect that the provider is in network. This is what patients and front desks see when they check whether a provider accepts a given plan.
Directory updates do not always happen immediately after approval. There can be a lag of days or weeks between when a provider is approved and when they show up accurately in a payor’s directory. That lag can cause confusion for patients and staff even when everything behind the scenes is technically in order.
Your effective date is the date the payor officially recognizes your participation. Services before that date are generally not covered under that plan, regardless of when the application was submitted or approved.
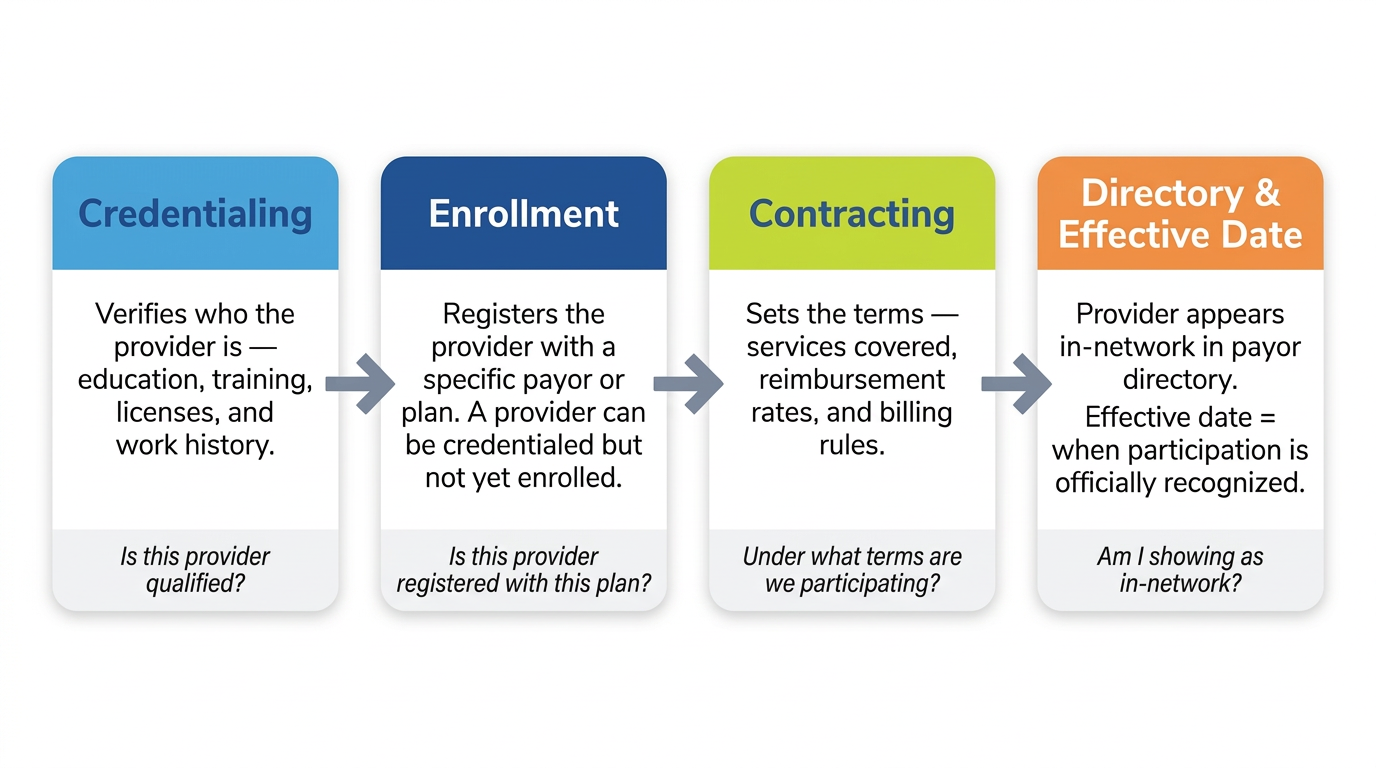
Why this matters for planning
Because these are separate steps, a delay in any one of them can hold up everything that follows. A provider can finish credentialing but still be waiting on enrollment. Enrollment can be approved but contracting terms not yet finalized. Everything can be done but the directory not yet updated.
This is why “are we in network?” is not always a simple yes or no. The real answer is: “credentialed with this payor, enrolled under this plan, contracted under these terms, and listed correctly in this directory.”
When you understand the full chain, you can track where things actually stand instead of waiting for a single “you’re approved” moment that may never come as one clear signal.
One brand, many plans
It is also worth knowing that most major insurance companies are not a single network. Under one brand, you can find employer plans, marketplace plans, Medicare Advantage plans, Medicaid managed care plans, and more. Each of those products can have its own credentialing requirements, enrollment pathways, and contracting terms.
This is how a provider ends up in network for some patients with a given insurance card but not others. Being enrolled with UnitedHealthcare commercial does not automatically mean you are enrolled in their Medicare Advantage or Medicaid products. Each requires its own application and approval.
When you are building a payor mix, the question is not just “which insurance companies do we want to work with?” It is “which specific products, under which entities, for which patient populations?”
At pie Health, we map this out at the start of every engagement so you know exactly what you are enrolled in, under what terms, and what gaps still exist. If you want to talk through how this applies to your practice, we are always glad to help.



