Credentialing Starts With the Right Payors
Avoid closed panels, low reimbursement, and wasted time. Get clarity before you commit—so every credentialing step counts.

What Happens During Payor Discovery
This is where strategy turns into action. For every payor you’re considering, we dig deeper to uncover key details before enrollment begins.
- Panel status to confirm if the payor is accepting new providers
- Fee schedule access and when it’s made available
- Contracting entity details and whether it’s direct or delegated
- Network placement and how you’d be listed for referrals
- Known issues with delays, blackout periods, or denials
- Pre-enrollment requirements like forms or extra verifications
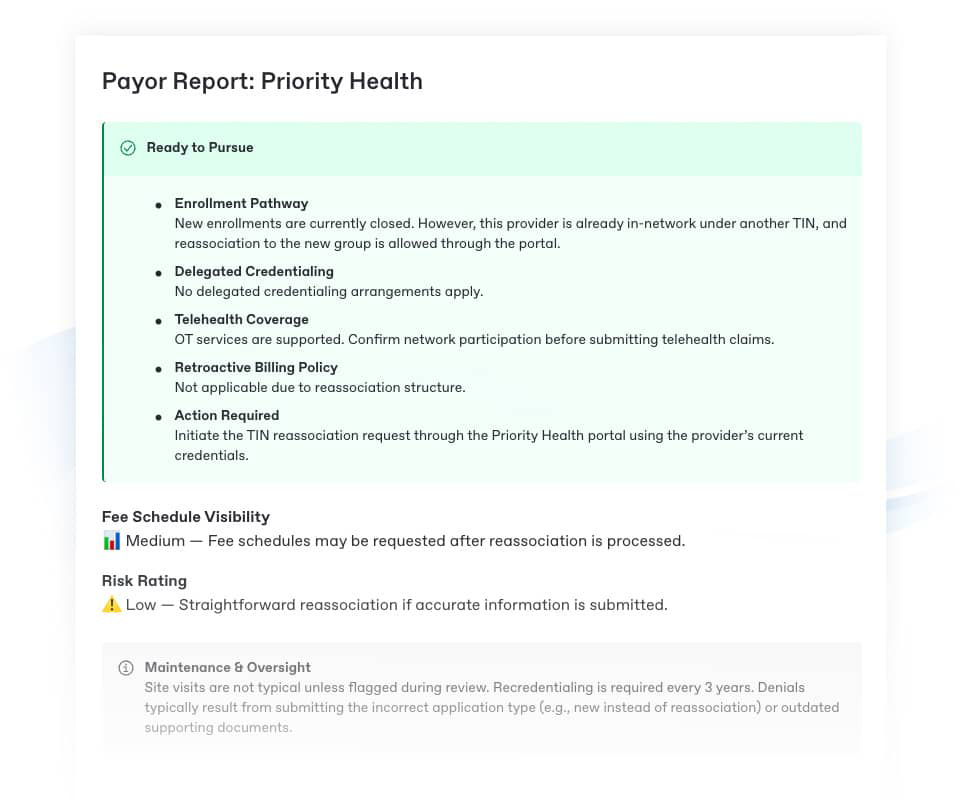
Less Risk. Better Decisions.
You won’t find this anywhere else. This is enterprise level credentialing strategy built for private practices and priced like it.
Clarity
Know which payors are actually open to providers in your specialty and state.
Transparency
Understand how each payor handles contracting, networks, and visibility.
Insight
Learn what others miss, like reimbursement risks and known processing delays.
Control
Avoid wasted effort on closed panels or non-viable enrollment paths.
Efficiency
Move forward only with payors that are likely to credential and pay fairly.
Confidence
Start the enrollment process with fewer surprises and stronger positioning.
Smarter Payor Enrollment Starts Here
We handle credentialing and payor enrollment with expert support, smart systems, and a personal touch.
Free Consultation
Start with a free call to share your goals, ask questions, and explore your options.
Credentialing Launch Plan
Get a strategic enrollment plan tailored to your market and specialty.
Credentialing Payor Discovery
See which payors are available and what’s needed to enroll.
Credentialing Dashboard
Track every step with your own real-time credentialing portal.